Comparing psychedelic and meditation-related adverse events
Plus other interesting links from around the internet
Welcome to Tuesday Brunch, the weekly round-up of interesting links. First bit is free.
How similar are psychedelic-related adverse events to meditation-related psychedelic events? You’d think sitting down quietly and counting your breath was quite different to getting blasted into elf-infested hyperspace on DMT. And yet there are interesting parallels. Now research is beginning to explore them.
When my colleagues and I launched the Challenging Psychedelic Experiences Project in 2022 to investigate post-psychedelic extended difficulties, we consciously followed in the foot-steps of meditation-related adverse event research. This field was pioneered by Dr Willoughby Britton and the team at Brown University and Cheetah House (an NGO Dr Britton set up to help those struggling with severe post-meditation difficulties).
I remember seeing Dr Britton present at a 2014 Mind and Life conference, and writing about it, 12 years ago. They published their first paper on meditation AEs (adverse events) in PLOS One in 2017 and have since published a tonne of papers on different kinds of harms, treatments, trauma-informed meditation, and so on.
Our 2023 study on extended post-psychedelic difficulties was consciously modelled on their first paper (we even published it in the same journal). Subsequent papers focused on specific types of difficulty (such as post-psychedelic existential confusion), just as they had done. They provided a really useful precedent for us.
There’s still a lot of work to be done comparing post-psychedelic and post-meditation adverse events, and Dr Britton is now working with others, especially her former PhD student Roman Palitsky, now at Emory, on a new study comparing post-psychedelic and post-meditation difficulties (if you’ve experienced either, you can take part in their study here:
What are the parallels? Well, people sometimes experience similar sorts of symptoms after both psychedelics and meditation - increased anxiety, derealisation and depersonalisation, somatic issues, sleep issues, PTSD, ontological shock (HPPD is apparently more confined to psychedelic users). There seems to be a similar prevalence - maybe as much as 40% of people experience some adverse event after both psychedelics and meditation, but it’s usually mild and transient, while around 8% may experience more disruptive and enduring difficulties.
Could there be a similar mechanism or mechanisms at work in both sorts of adverse event? It’s possible. I asked Daniel Ingram, meditation expert and founder of the Emergent Phenomena Research Collective, what he thought. He said:
I would be amazed if the mechanisms didn’t have a great deal of overlap, some of the same core processes, mechanisms, receptors, pathways, developmental issues, etc. Lots of the same phenomenology, stories often sound very similar, similar things help, similar things harm in similar ways, trajectories often quite similar, etc. This will need to be disentangled with better science than my 30+ years of talking to thousands of people about both (often in the same people), but that is my strong conclusion so far.
Both psychedelics and meditation, of course, alter consciousness, sometimes in profound ways. As Daniel once said to me: ‘People alter their consciousness intentionally. Sometimes they come back to the same place they were before, sometimes they land in a better place or even a much better place, and sometimes they land in a worse place.’
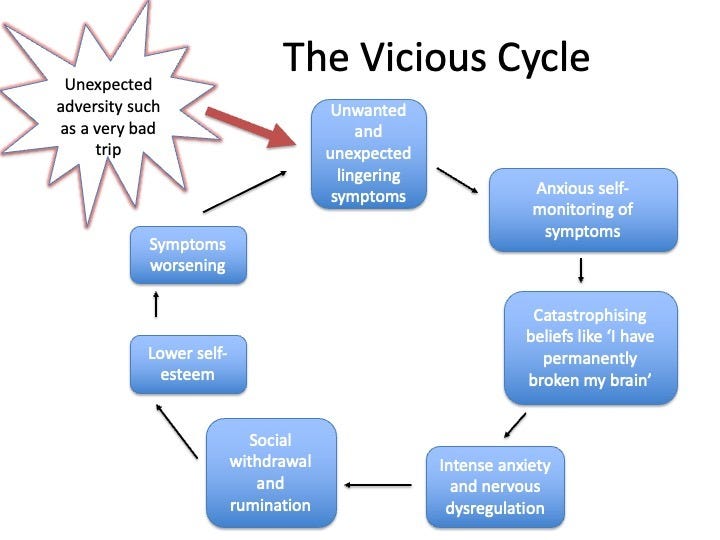
I wonder if there’s a cognitive behavioural process at work after both difficult meditation experiences and difficult trips. There’s an adverse event, a trigger, which creates unexpected and unwanted mental, emotional and physical symptoms. For most people they pass after a few days, but some people get stuck in a cycle of anxiety, catastrophising and hyper-vigilant self-monitoring. Each time the unwanted symptom occurs, they think ‘here it is again, this proves my brain is permanently broken’ (this catastrophic belief is very common in people with extended post-psychedelic difficulties, and Roman Palitsky tells me it’s also very common in people with meditation-related difficulties). Then people can ruminate more and more on their inner state, they feel shame, despair and lower self-esteem, and they can withdraw from life - a tactical mistake as this just increases rumination, depression and lower self-esteem. It’s a vicious cycle that people can be stuck in for years, as I was.
With both meditation and psychedelics, there’s also a cultural context of massive hype, and perhaps this increases the unexpectedness and unwantedness of unpleasant after effects: ‘what the hell is this? I didn’t sign up for this! This was supposed to be healing. I was expecting to feel better’.
Check out the video of our event on (ex) Mormons and Psychedelics.
For some people (including me), a Cognitive Behavioural / Acceptance and Commitment Therapy framework can be helpful: Accepting the adverse event that happened, accepting the difficult symptoms when they arise and letting them pass away rather than fixating on them, cognitive reframing of catastrophising beliefs, relaxing and calming the body, social support / normalisation of what you’re going through / hope that recovery is possible; and finally, re-engagement with life and what gives you meaning and joy.
But that’s just one frame. As Matthew Sacchet and colleagues at Harvard highlight in an interesting new paper on post-meditation difficulties, there are many possible explanatory frameworks or worldviews for such difficulties. For some intense meditators, they’re an expected and accepted part of the contemplative path to enlightenment - the ‘stage of arising and passing away’, as Daniel Ingram calls it, or the dark night of Christian mysticism. For other people, according to Sacchet, such disturbances are within their ‘window of arousal’, so they can accept them without being overly disturbed. Likewise, there are a bunch of different ways people can interpret and respond to post-psychedelic difficulties - ‘spiritual emergency’, ‘kundalini awakening’, ‘spirit possession or curse’, ‘psychiatric crisis’, ‘integration challenge’, ‘trauma resurfacing’, and so on. It would be useful to map all these possible meaning-and-response frameworks, but I’ll leave that for a future post.
In general, research into adverse events is often ignored and underfunded - who wants to fund that? Research into talk therapy adverse events is extremely limited, research into SSRI adverse events is underfunded, research into Transcranial Magnetic Stimulation adverse events barely exists, likewise for ketamine treatments. Often, adverse event research starts with lone voices posting their distress on social media, then slowly, social media groups form to share stories of severe adverse events, the industry initially ignores them, until gradually their stories coalesce into data and make their way into academic studies, or possibly law cases, finally feeding back into industry safeguards, or law-suits.
The research into meditation adverse events is about eight years ahead of psychedelics, and there’s a lot we can learn from them. As for AI-related adverse events, the field is only just beginning - we don’t even know what harms people experience, or how often, yet.
After the paywall, the WSJ has a big piece on ketamine adverse events; plus new papers on AI delusions and the perils of AI sycophancy; an Oregon man sentenced to 20 years for killing his wife on LSD; Trump’s surprising popularity as he disrupts Latin America; and a psychedelic horror story created by Claude.